MASSIVE CELL: Colored transmission electron micrograph of a macrophage cell, one of the largest cells in the body© MEDIMAGE/SCIENCE SOURCE
MASSIVE CELL: Colored transmission electron micrograph of a macrophage cell, one of the largest cells in the body© MEDIMAGE/SCIENCE SOURCE
In the mid-1990s, while researching mice’s immune responses to nematode worms, immunoparasitologist Judi Allen of the University of Manchester spotted macrophages accumulating at the site of a multicellular parasite infection.1 This was unexpected, she told The Scientist; at the time, the immune cells were only known for their antimicrobial activity—a different type of immune response from that known to fight large parasitic worms. The mystery continued, as RNA sequencing revealed that the immune cells’ gene expression differed greatly from that of macrophages activated by a microbial infection.2 “It was so shockingly different that we were thrown,” says Allen. “It didn’t tell us at all what these macrophages were doing, because the list of genes that they were [expressing] were completely unknown.”
Only years later, when...
For more than a century, macrophages—which means “big eaters” in Greek—were considered relatively simple cells whose sole job was to engulf bacteria, other microbes, and cellular debris. Averaging around 20 μm across in humans, they are among the largest cells in the body, which helps them to physically surround and digest their microscopic meals. “You can think of them as the vacuum cleaners of the body,” Babak Razani, a physician and researcher at Washington University School of Medicine in St. Louis, writes in an email.
But over the last 10 years, research has demonstrated that this is only part of the picture. In terms of immune defense, investigators now understand that macrophages mount a three-stage response to infection. “Their initial role when our body is invaded with a pathogen is a more inflammatory-and-defense function,” says Sourav Ghosh, a biologist at Yale University School of Medicine. Macrophages stimulate inflammation and release a cocktail of molecules to kill microbes. After engulfing a pathogen, macrophages keep hold of pieces of the invader’s proteins, known as antigens, and present these to T cells.
With the advent of single-cell genomics, we’re in a moment when we can actually look at individual subtypes of macrophages, and we’re finding that there is an enormous heterogeneity amongst them.—Nadia Rosenthal, Jackson Laboratory
In the final stage of macrophages’ response to infection, “they will take on a resolving phenotype, where they produce a variety of anti-inflammatory factors that help quiet the inflammation,” says Tom Wynn, an immunologist at the National Institute of Allergy and Infectious Diseases. It is during this stage that macrophages stimulate repair of the damage to surrounding tissues, by releasing growth factors and signaling fibroblasts to spring into action and seal the wound.4 “Macrophages appear to orchestrate the repair as well as to initiate it,” says Nadia Rosenthal, a regeneration biologist at the Jackson Laboratory in Maine. “The anti-inflammatory phase is accompanied by a gene expression shift into a more proregenerative profile.”
As researchers have begun to take a closer look at these underestimated cells, they have also recognized roles for macrophages outside of immunity. For example, the cells are involved in directing tissue development, transporting chemical messages, even regulating body weight and conducting electrical impulses. “With the advent of single-cell genomics, we’re in a moment when we can actually look at individual subtypes of macrophages, and we’re finding that there is an enormous heterogeneity amongst them,” explains Rosenthal.
“I think we’re learning [that] more and more cells in the body are much more flexible . . . than we originally thought,” says Wynn. “Macrophages are probably exceptional in that ability.”
 MACROPHAGES AROUND THE BODY: Tissue-resident macrophages, which not only respond to local assaults but also function in normal development and physiology, originate in the yolk sac of the embryo and mature in one particular tissue in the developing fetus, where they acquire tissue-specific roles and change their gene expression profile. By contrast, circulating macrophages are produced throughout life by the bone marrow, then released into the vasculature to respond to infections and injury.
MACROPHAGES AROUND THE BODY: Tissue-resident macrophages, which not only respond to local assaults but also function in normal development and physiology, originate in the yolk sac of the embryo and mature in one particular tissue in the developing fetus, where they acquire tissue-specific roles and change their gene expression profile. By contrast, circulating macrophages are produced throughout life by the bone marrow, then released into the vasculature to respond to infections and injury.
See full infographic: WEB | PDF© SCOTT LEIGHTON
Tissue repair
The complexity of the wound-healing process and macrophages’ role in it is only just starting to emerge. In a study published in Science this May, Ghosh, immunologist Carla Rothlin of Yale University School of Medicine, and their colleagues showed that macrophages integrate multiple signals from their local environment to produce a tailored response to infection and injury.5 Cytokines recruit more macrophages to the site of inflammation, but these signaling molecules alone are not sufficient to initiate the wound-healing process. “Macrophages can sense cells that die in the tissue, and they can integrate this sense to induce a tissue-repair response,” says Rothlin. In the same issue of Science, Allen and her colleagues announced the discovery of tissue-specific signals needed to activate macrophages in the lung and liver to repair damaged tissue.6
See “Newly Discovered Emergency Responders to Liver Damage”
Tissue repair doesn’t always go smoothly, however. In chronic injuries, conflicting signals can confuse macrophages into activating all three stages of their response at once. “You can have macrophages that are at the proinflammatory stage of activation, macrophages that are pro-wound healing, and macrophages that exhibit some pro-resolving activities, all at the same time,” leading to wounds that simply won’t heal, explains Wynn.
Other times, wounds do heal, but the injuries leave a scar. Internal scarring, also known as fibrosis, is a hardening of tissues that occurs when macrophages stimulate fibroblasts, which synthesize the extracellular matrix, to produce too much collagen during the repair process. Scar tissue is at the root of many diseases, including liver cirrhosis, and cardiovascular and kidney diseases. “Fibrosis is one of the biggest challenges in Western medicine—that’s what most people end up dying of,” says Allen.
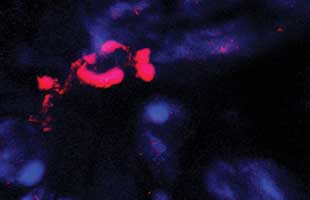
 Macrophages (red) at the wound site in spiny mouse ear tissue five days after injury. (Scale bar = 10 micrometers)JENNIFER SIMKIN Perhaps nowhere in the body is the ability to repair damaged tissue more important than in the heart. Although fetal mammals are typically able to regenerate heart tissue without scarring, most species lose that ability as adults, for reasons scientists still don’t fully understand. Studying heart repair in mouse fetuses, researchers have learned that, while macrophages are often responsible for the development of fibrosis in adults, they also play a starring role in scar-free repair. Kory Lavine, a researcher and cardiologist at Washington University School of Medicine, suggests that the difference may be attributed to where the macrophages come from.
Macrophages (red) at the wound site in spiny mouse ear tissue five days after injury. (Scale bar = 10 micrometers)JENNIFER SIMKIN Perhaps nowhere in the body is the ability to repair damaged tissue more important than in the heart. Although fetal mammals are typically able to regenerate heart tissue without scarring, most species lose that ability as adults, for reasons scientists still don’t fully understand. Studying heart repair in mouse fetuses, researchers have learned that, while macrophages are often responsible for the development of fibrosis in adults, they also play a starring role in scar-free repair. Kory Lavine, a researcher and cardiologist at Washington University School of Medicine, suggests that the difference may be attributed to where the macrophages come from.
 Macrophages (red) emerge from a blood vessel (red blood cells stained in yellow) at the wound site five days after injury in spiny mouse ear tissue. (Scale bar = 10 micrometers)JENNIFER SIMKINIn addition to the well-studied circulating macrophages (often called monocytes) that are produced in the bone marrow and are released into the blood to patrol for and respond to infection, in the 1980s researchers began to recognize that some macrophages are produced from embryonic stem cells during early development and remain permanently within one tissue. “The biggest revolution in macrophage biology in the past five years has been this understanding that macrophages that live in the tissues are quite fundamentally different than macrophages that circulate in the blood,” explains Allen.
Macrophages (red) emerge from a blood vessel (red blood cells stained in yellow) at the wound site five days after injury in spiny mouse ear tissue. (Scale bar = 10 micrometers)JENNIFER SIMKINIn addition to the well-studied circulating macrophages (often called monocytes) that are produced in the bone marrow and are released into the blood to patrol for and respond to infection, in the 1980s researchers began to recognize that some macrophages are produced from embryonic stem cells during early development and remain permanently within one tissue. “The biggest revolution in macrophage biology in the past five years has been this understanding that macrophages that live in the tissues are quite fundamentally different than macrophages that circulate in the blood,” explains Allen.
It is these tissue-resident macrophages that contribute to repair in the neonatal heart, Lavine says, explaining that “macrophages [from the blood] really don’t enter the heart until the postnatal period.” In fact, the resident macrophages appear to actively keep the circulating monocytes out of the developing heart, Lavine adds.7 Removing the resident macrophages from the heart in neonatal mice results in inflammation and scar-tissue formation.8
Just as macrophages seem essential for setting up a blood supply for developing organs, they are also complicit in helping tumors develop.
In adults, on the other hand, the tissue-resident macrophages are depleted after an initial heart injury and circulating monocytes are recruited to replace them, Lavine’s group found.9 These recruited macrophages cause inflammation and tissue damage as they force their way between cells, which may prevent successful tissue regeneration and lead to scarring. In the heart, says Rosenthal, recruited “macrophages do not appear to be able to make that transition to a proregenerative state; [they] continue to be proinflammatory.”
|
REGROWING LOST LIMBS
In 2013, for example, Nadia Rosenthal of the Jackson Laboratory and colleagues reported that macrophages were essential for successful limb regeneration in the axolotl (Ambystoma mexicanum).10 “The first five days of wound healing [in most organisms] involves a stately procession of different components of the immune system, which arrive like clockwork at the site of the injury,” Rosenthal says. But not so in a regenerating axolotl limb. “Within 24 hours, every cell type that we can identify in the salamander’s immune system is on board at that site,” suggesting a very rapid progression of normal wound healing factors and the speedy resolution of the inflammatory phase, she says. At a localized level, some mammals can also regenerate tissues such as the skin or the tips of their fingers and toes, and macrophages appear to have a hand in such smaller-scale regenerative activities as well. One unique mammal, the African spiny mouse (Acomys cahirinus), is capable of regenerating complex tissue in the fleshy part of the ear, including cartilage, hair follicles, and sweat glands.11 In May, University of Kentucky regeneration biologist Ashley Seifert and his team showed that removing macrophages during injury prevented normal regeneration in the spiny mouse.12 During tissue repair and regeneration, “we think the different immune cell types help facilitate activation of local fibroblasts,” Seifert explains. Fibroblasts, under the direction of macrophage-produced signals, can form extracellular structures that act as scaffolding during the repair process. |
Development
Since discovering permanent tissue populations of macrophages, researchers have noted that they appear to be important for the normal development of many tissues. Last year, for example, Lavine and colleagues found that resident macrophages actively shape the development of blood vessels in neonatal mouse hearts. In a growing fetus, blood vessels form a network of capillaries that cover the heart before blood has even begun to flow through them. After blood flow is connected, Lavine’s group found, macrophages are attracted to vessels with the highest flow and release molecules that promote their growth. The cells also release signals that direct blood vessels receiving little blood flow to recede, trimming the branching blood vessel network.13
A similar process also guides neurons and blood vessels in the developing brain. Resident macrophages in the brain, known as microglia, populate the organ during embryonic development, producing growth factors for neurons and coordinating synaptic pruning—both essential processes for normal brain development. “[Microglia] set up a completely independent population of self-renewing cells,” separated from macrophages in the rest of the body by the blood-brain barrier, says Chris Glass, a molecular immunologist at the University of California, San Diego School of Medicine.
 CELLULAR VACUUM CLEANERS: For years, macrophages were recognized only for their roles in gobbling up cellular debris, dead cells, and bacteria, such as the Mycobacterium tuberculosis shown here in pink.© SPL/SCIENCE SOURCE
CELLULAR VACUUM CLEANERS: For years, macrophages were recognized only for their roles in gobbling up cellular debris, dead cells, and bacteria, such as the Mycobacterium tuberculosis shown here in pink.© SPL/SCIENCE SOURCE
Further evidence for macrophages’ role in the development of the brain and its vasculature came earlier this year, when neurobiologist Ana Martin-Villalba at the German Cancer Research Center (DKFZ) and colleagues found that a macrophage-produced protein called CD95L binds to CD95 receptors on the surface of neurons and developing blood vessels in the brains of mouse embryos. The CD95 receptor and its ligand are best known for triggering cell death, or apoptosis, in response to viral infections, cancers, and stressors, such as free radicals and oxygen deprivation. Without CD95L, Martin-Villalba’s team showed, neurons branched less frequently, and the resulting adult brain showed less electrical activity.14 “In the developing brain the macrophages, just using one signal, are shaping the developing neurons and vessels at the same time,” she says.
But just as macrophages seem essential for setting up a blood supply for developing organs, they are also complicit in helping tumors develop. “Cancer is nothing [but] a developing organ,” explains Martin-Villalba. “Normally, if you find something going on in development, it’s pretty much the case that you find this very same issue in cancer.”
Developing tumors attract circulating monocytes from the blood and stimulate the immune cells to become tumor-associated macrophages. When the process goes smoothly, these macrophages kill tumor cells and release factors to destroy their blood supply. But when things go wrong, they instead produce growth factors that help the developing tumor grow its network of blood vessels, just as macrophages do for developing organs in a fetus.
The link between macrophages and cancer was first identified in the 1860s, when German physician Rudolf Virchow noted that cancer was often associated with inflammation. But it wasn’t until the 20th century that his ideas were taken seriously, as researchers began to find loads of the cells in biopsied tumors. Researchers now know that some 15 percent of cancers are triggered by infection, which can jump-start the inflammatory process. Macrophages are also found at the site of cancers caused by other factors, such as carcinogens or genetic mutations, and cancer initiation and progression has been linked to chronic inflammation.15 “The most aggressive types of cancer have the highest infiltration of macrophages and other immune cells,” says Martin-Villalba.
Researchers have long known that CD95L, also known as the death protein for its role in apoptosis, is expressed by certain immune cells to trigger the process in cancer cells. But tumors can become resistant to CD95L’s apoptotic effects. In addition to preventing cancer cell death, this resistance might also help tumors survive and develop by promoting blood-vessel growth, Martin-Villalba suggests. “We postulate that macrophages in a brain tumor can produce signals like CD95L that act on vascularization of the tumor,” she says. During Phase 2 clinical trials in 2012, she and her colleagues found increased overall survival in one group of CD95L-expressing brain tumor patients when treated with a protein compound that binds CD95L to prevent it from activating CD95 receptors.
It is now eminently clear that macrophages are far more than the garbage disposals scientists first viewed them as.
Macrophages may also be involved in a host of neurodegenerative diseases and psychiatric illnesses. Earlier this year, Glass and colleagues analyzed the transcriptomes of microglia from 19 patients undergoing brain surgery, and found that many genes containing risk variants previously associated with diseases such as Alzheimer’s, Parkinson’s, schizophrenia, and multiple sclerosis were more highly expressed in microglia than in other cells in the brain.16 For instance, 58 percent of genes known to influence the risk of developing Alzheimer’s disease were expressed at levels at least 10 times greater in the microglia than in cortical tissue. This suggests that these genetic variants may increase the risk of disease for patients carrying them by affecting the action of microglia in the brain.
Within hours of being removed from the brain and cultured in the laboratory, however, the microglia had completely changed their expression profile, reducing transcript levels of more than 2,000 genes. Their ability to rapidly change according to environmental conditions might have important implications for scientists studying microglia, making it difficult to generalize from cell-culture studies to macrophages in vivo.
As macrophages’ role in development is further elucidated, researchers may uncover additional ways the cells mediate both health and disease. (See “Medicinal Reprogramming.”) For example, monocyte-derived cells known as osteoclasts are involved in bone development, and mice that lack these cells develop dense, hardened bones—a rare condition known as osteopetrosis. Macrophages also orchestrate development of the mammary gland and assist in retinal development in the early postnatal period.17 The next step, says Glass, will be to “carefully evaluate the consequences of removing macrophages from specific tissues during development and asking what the consequences are [for] the development of that tissue.”
Homeostasis
Beyond their roles in development and wound healing, macrophages are now recognized for their important functions in maintaining the status quo in the adult body. Tissue macrophages are highly sensitive to changing conditions, and respond by releasing cell signaling molecules that trigger a cascade of changes allowing cells to adapt. For instance, macrophages in adipose tissue regulate the production of new fat cells in response to changes in diet or exposure to cold temperatures. Macrophages in the liver, known as Kupffer cells, regulate the breakdown of glucose and lipids in response to dietary changes, and have been linked to obesity and diabetes. “Nowadays they are recognized as major sentinel cells that can sense changes in tissues,” says Rothlin.
See “Fat’s Immune Sentinels”
In the testis, macrophages help create a protective environment for sperm. Sperm cells are at risk of attack by the immune system because they are first produced during puberty, after the immune system has developed. Their specific antigens might be accidentally flagged as foreign, but tissue-resident macrophages in the testis produce immunosuppressant molecules that guard against this.18
Macrophages also appear to be critical for the function of the heart. Research has revealed that resident macrophages are present in large numbers, “close to the structures that conduct electricity in the heart,” explains Matthias Nahrendorf, a cardiovascular physician at Massachusetts General Hospital’s Center for Systems Biology. Curious about the role of these macrophages, Nahrendorf and colleagues at Harvard Medical School engineered mice that lacked them. Unexpectedly, they found that the rodents developed a condition known as an AV block, which inhibits conduction of electricity in the heart, and in humans is usually treated with a pacemaker.19 “That was a big surprise to me,” he says. Without macrophages, “the electrical impulse was not able to travel from the atrium to the ventricle.”
Indeed, when they measured the membrane electrical potential of macrophages and cardiomyocytes, the researchers found the cells are directly involved in conducting electricity, polarizing and depolarizing rhythmically to help keep the heart beating regularly. “That was the other big surprise for me,” Nahrendorf says—“that there’s really electrical connection and cross talk between macrophages and cardiomyocytes.” Rosenthal was similarly taken aback. The role of macrophages in electrical conduction “was a complete shock,” she says.
It is now eminently clear that the cells are far more than the garbage disposals scientists first viewed them as. “I think the immunologists are staring in disbelief at the armada of nonimmunological laboratories that have suddenly realized that they’re going to have to acknowledge the omnipotence of the immune system and how complicated it is,” says Rosenthal. “And I’m one of them; I’m a convert.”
|
Given macrophages’ ever-expanding role in normal development and physiology as well as disease, perhaps it should be no surprise that researchers are now eyeing the cells as potential targets for various therapies. One potential application may be in treating atherosclerosis, plaque build-up in the arteries that can result from inflammatory macrophages engulfing excess lipids. The cells eventually become lipid-engorged, and these “obese macrophages,” as Babak Razani of Washington University School of Medicine calls them, tend to stimulate more inflammation and recruit more macrophages, clogging the circulatory system and heart with plaque. But Razani believes he may have found a clever trick to improve macrophages’ ability to play a more positive role. This June, Razani and his colleagues showed that macrophages in the blood vessels can be stimulated with a common sugar molecule to become “super macrophages,” with an enhanced ability to degrade plaque.20 Trehalose, a disaccharide, changes macrophage gene expression, causing the cells to carry more digestive organelles called lysosomes, and resulting in a 30 percent decrease in atherosclerotic plaque in mice injected with trehalose. “Trehalose is a safe and natural sugar, already being used in many pharmaceuticals and being consumed as a sweetener,” Razani says. But he warns a healthy heart is not as simple as just adding more sweeteners to your tea. When consumed in the diet, the enzyme trehalase quickly breaks down trehalose into the simple, nontherapeutic sugar, glucose. The next step towards a medicinal application of this research will be to find ways to deactivate trehalase, so that trehalose can make it into the bloodstream undigested, ready to unleash its macrophage-enhancing powers. Other potential medical applications for macrophages could include manipulating the cells to promote healthy scar-free wound repair. This might involve devising ways to keep macrophages in the blood from being called in to deal with heart damage, or reprogramming stem cells into wound-healing macrophages that could be injected at the site of a chronic wound. “We don’t just want to turn them off in pathological conditions,” says biologist Jennifer Simkin, a postdoc at the University of Kentucky. “Instead, we want to try and control what they’re secreting and what they’re doing.” First, however, researchers must continue to interrogate the cells’ basic biology. A better understanding of their roles in health and disease, as well as their therapeutic potential, may then follow, says Razani. “[An] integrative approach to studying [macrophages] will yield long-term dividends in understanding fundamental biological processes, unraveling mechanisms of disease, and eventually modulating their function to treat human disease.” |
Claire Asher is a freelance science writer living in London, U.K.
References
- P. Loke et al., “Alternatively activated macrophages induced by nematode infection inhibit proliferation via cell-to-cell contact,” Eur J Immunol, 30, 2669-78, 2000.
- P. Loke et al., “IL-4 dependent alternatively-activated macrophages have a distinctive in vivo gene expression phenotype,” BMC Immunol, 3:7, 2002.
- P. Loke et al., “Alternative activation is an innate response to injury that requires CD4+ T cells to be sustained during chronic infection,” J Immunol, 179, 3926-36, 2007.
- T.A. Wynn, K.M. Vannella, “Macrophages in tissue repair, regeneration, and fibrosis,” Immunity, 44:450-62, 2016.
- S. Ghosh et al., “Macrophage function in tissue repair and remodeling requires IL-4 or IL-13 with apoptotic cells,” Science, 356:1072-76, 2017.
- C.M. Minutti et al., “Local amplifiers of IL-4R–mediated macrophage activation promote repair in lung and liver,” Science, 356:1076-80, 2017.
- S. Epelman et al., “Embryonic and adult-derived resident cardiac macrophages are maintained through distinct mechanisms at steady state and during inflammation,” Immunity, 40:91-104, 2014.
- A.B. Aurora et al., “Macrophages are required for neonatal heart regeneration,” J Clin Invest, 124:1382-92, 2014.
- K.J. Lavine et al., “Distinct macrophage lineages contribute to disparate patterns of cardiac recovery and remodeling in the neonatal and adult heart,” PNAS, 111:16029-34, 2014.
- J.W. Godwin et al., “Macrophages are required for adult salamander limb regeneration,” PNAS, 110:9415-20, 2013.
- T.R. Gawriluk et al., “Comparative analysis of ear-hole closure identifies epimorphic regeneration as a discrete trait in mammals,” Nat Commun, 7:11164, 2016.
- J. Simkin et al., “Macrophages are necessary for epimorphic regeneration in African spiny mice,” eLife, 6:e24623, 2017.
- J. Leid et al., “Primitive embryonic macrophages are required for coronary development and maturation,” Circ Res, 118:1498-511, 2016.
- 1S. Chen et al., “CNS macrophages control neurovascular development via CD95L,” Cell Rep, 19:1378-93, 2017.
- A. Mantovani et al., “Cancer-related inflammation,” Nature, 454:436-44, 2008.
- D. Gosselin et al., “An environment-dependent transcriptional network specifies human microglia identity,” Science, 356:eaal3222, 2017.
- 1T.A. Wynn et al., “Macrophage biology in development, homeostasis and disease,” Nature, 496:445-55, 2013.
- N. Mossadegh-Keller et al., “Developmental origin and maintenance of distinct testicular macrophage populations,” J Exp Med, 214:10.1084/jem.20170829, 2017.
- M. Hulsmans et al., “Macrophages facilitate electrical conduction in the heart,” Cell, 169:510-22.e20, 2017.
- I. Sergin et al., “Exploiting macrophage autophagy-lysosomal biogenesis as a therapy for atherosclerosis,” Nat Commun, 8:15750, 2017.
Interested in reading more?