 WILDLIFE DISEASE: A European rabbit (Oryctolagus cuniculus) suffering from myxomatosis.© JOE BLOSSOM/ALAMY STOCK PHOTO
WILDLIFE DISEASE: A European rabbit (Oryctolagus cuniculus) suffering from myxomatosis.© JOE BLOSSOM/ALAMY STOCK PHOTO
 A house finch (Haemorhous mexicanus) infected with the bacterium Mycoplasma gallisepticum.ANDY DAVIS, UNIVERSITY OF GEORGIAOne of the most remarkable events in the history of infectious diseases began at the end of 1950. A smallpox-like virus that was being trialed as a biological control agent for the invasive rabbit populations in Australia escaped from test sites and caused an outbreak of unprecedented scale, speed, and carnage. Within just six months, it had spread up the river systems in four states and was decimating rabbit populations across a million square miles. “In places it was possible to drive for a day or more through country that had previously been swarming with rabbits and see only isolated survivors,” one research team reported.1 Tens, perhaps hundreds, of millions of rabbits...
A house finch (Haemorhous mexicanus) infected with the bacterium Mycoplasma gallisepticum.ANDY DAVIS, UNIVERSITY OF GEORGIAOne of the most remarkable events in the history of infectious diseases began at the end of 1950. A smallpox-like virus that was being trialed as a biological control agent for the invasive rabbit populations in Australia escaped from test sites and caused an outbreak of unprecedented scale, speed, and carnage. Within just six months, it had spread up the river systems in four states and was decimating rabbit populations across a million square miles. “In places it was possible to drive for a day or more through country that had previously been swarming with rabbits and see only isolated survivors,” one research team reported.1 Tens, perhaps hundreds, of millions of rabbits...
To everyone’s delight, the carnage continued, helped by subsequent deliberate releases in other parts of Australia. Over the ensuing decade, rabbit populations in wide swaths of the country were reduced to a tenth of what they had been.2 Since that time, rabbit populations have rebounded somewhat, but are nowhere near what they once were. The culpable agent, myxoma virus (MYXV), has generated billions of dollars of savings for Australian agricultural industries to date,3 surely one of the most cost-effective interventions in the history of agriculture.
The episode also presented a unique opportunity to study the evolutionary arms race between a pathogen and its host animal. Australian microbiologist Frank Fenner took advantage, setting up just the right experiments at just the right time—and he and colleagues kept them going for more than 35 years.4 The body of work he produced and inspired in others has generated a detailed view of the evolution that ensues when a virus emerges in a new host population.2 In the process, it also offers important insights into how pathogens might react when interventions such as vaccination and genetic engineering make hosts more resistant to their infections—an important ambition in agricultural and human medicine.
Viral virulence
In fully susceptible rabbits, the strain of MYXV that started it all causes classical myxomatosis, a nasty disease in which the eyes, ears, and genitals swell and then, as the eyes seal shut with discharge and the head begins to puff up, mucoid lesions develop on the skin. Almost every infected rabbit dies within two weeks. The question Fenner asked was: What happens when such a virulent virus spreads through a very susceptible host species on a continental scale? He focused on two possibilities. First, the highly lethal virus might evolve to become less lethal. Second, the highly susceptible rabbits might evolve resistance. Thanks to Fenner, we now know both happened.
We know of no cases where controlled experiments have shown declines in pathogen virulence in the face of rising host resistance.
Let’s start with the virus. It’s impossible to tell if a pathogen is getting more or less nasty by simply looking for changes in death rates: lots of things can contribute to a change in apparent virulence. Most obviously, hosts can acquire immunity or develop resistance, and so reduce disease severity without any genetic change in the pathogen. The only way to know for sure if a pathogen is evolving to be more or less nasty is to make comparisons in what is called a common garden, a standard setting that does not change. Fenner realized this immediately, and he soon began comparing the lethality of viruses isolated from the field in laboratory rabbits of the same species.4 (See illustration here.)
The work showed that the almost invariably lethal progenitor virus strain was replaced within a few years by strains with case fatality rates of 70 percent to 95 percent. Some field isolates killed fewer than half the lab rabbits. Over the next few decades, things settled down, and strains at both ends of the lethality spectrum become increasingly difficult to find. Fenner showed why. The highly lethal progenitor virus killed rabbits so fast that its infectious period was shorter than that of the less lethal viral mutants. That meant that the less lethal strains were able to infect more new victims and spread throughout the population.
Natural selection thus favored reductions in virulence. But it did not favor substantial reductions. Benign strains, it turned out, were also less infectious, this time because host immunity was able to control and clear them more rapidly. This work—the time series of isolates tested in a common garden and the experimental dissection of the relationship between virulence and transmission—made MYXV the poster child of virulence evolution: a highly lethal pathogen became less lethal over time. But it was still pretty nasty. It had not become benign.
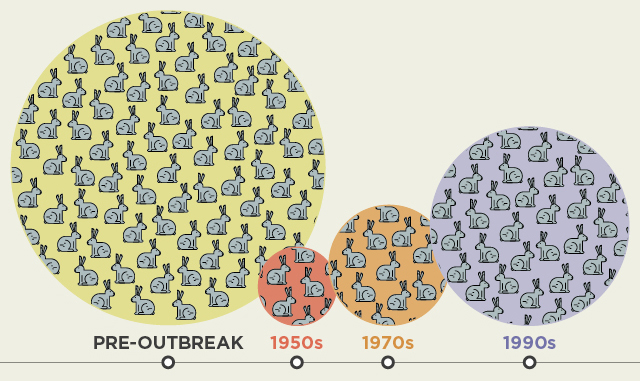 EVOLVING VIRULENCE: Tracking the myxoma virus in the wild rabbit populations of Australia has yielded insight into how pathogens and their hosts evolve.
EVOLVING VIRULENCE: Tracking the myxoma virus in the wild rabbit populations of Australia has yielded insight into how pathogens and their hosts evolve.
See full infographic: WEB | PDF
Escalation
In most textbooks, the story stops there. But the virus continued to evolve. From the late 1970s, reports began to accumulate that MYXV was becoming more lethal again. The picture was not simple, partly because the sampling was not as extensive as it had been during Fenner’s studies, and partly because there was substantial regional variation. Fascinated by the possibility that the textbook evolutionary trajectory of virulence had reversed, we, together with Eddie Holmes of the University of Sydney and Penn State University’s Isabella Cattadori, have been using Fenner’s common garden protocols to find out what happened.
To our great surprise, the most virulent of the isolates harvested from the field and frozen in the 1990s caused our susceptible laboratory rabbits to develop a highly lethal immune collapse syndrome akin to septic shock. This disease syndrome had never been seen before. Rabbits die at about the same rate as those infected with the ancestral virus, but they do so without developing classical myxomatosis. Instead, death is associated with a form of toxic or septic shock characterized by an almost complete absence of cellular inflammatory responses, allowing normally well-controlled bacteria to run rampant in the test rabbits. Evidently, sometime after Fenner’s detailed work, MYXV evolved the ability to very profoundly immunosuppress rabbits. From our phylogenetic and molecular-clock dating studies, our best estimate is that viral genes encoding this phenotype first arose sometime between the mid-1970s and the early 1980s.5
Why did the virus evolve in this way? The most likely explanation is that hyper-immunosuppression was MYXV’s answer to genetic resistance that evolved in wild Australian rabbits. Using the common garden approach but in reverse, this time experimentally infecting wild-caught rabbits with a control virus, Fenner and colleagues showed that genetic resistance had rapidly evolved in wild rabbit populations in the 1950s—hardly surprising given the devastation MYXV wreaked on rabbit populations and the fact that surviving rabbits can breed like, well, rabbits. The resistance that evolved clears MYXV infections more rapidly, and so reduces virus transmission. Importantly, resistance is not perfect: it does not prevent infection or transmission. The virus can thus evolve in resistant rabbit populations, and so any viral mutants that are better able to overcome enhanced antiviral host defenses will be favored by natural selection. Hyper-immunosuppression is precisely the sort of viral adaptation that could arise in such circumstances.
It is important to recall that we discovered the immune collapse when we tested viral strains in genetically susceptible lab rabbits. In the field, these same viral strains cause a classical myxomatosis presentation. Apparently, the net effect of hyper-immunosuppressive viruses in resistant wild rabbits is a disease syndrome not unlike the original. It is much like ducks staying calmly in place on a fast-flowing river: frantic paddling resulting in little change on the surface. Fenner’s common garden protocols make it possible to see what’s going on below the surface: the rabbits have become more resistant and, in turn, the viruses have evolved to suppress the host immune system on a large scale, allowing MYXV to continue to manifest the classical disease.
A common theme
 NASTY PATHOGENS: Infections that circulate among wild animals, such as the myxoma virus in rabbits or the bacterium Mycoplasma gallisepticum in house finches, tend to increase in virulence as hosts develop resistance. If the same holds true for farmed animals, there’s concern that breeding and vaccination efforts aimed at increasing host resistance could fuel the evolution of more virulent pathogens. Chris Cairns (bottom, left) and Andrew Read of Penn State University are studying this phenomenon, pictured here sampling broiler chickens for Marek’s disease virus in central Pennsylvania.RABBIT: PETER KERR; FINCH: BOB VUXINIC; CHICKENS: ASHLEY CHANCommon garden experiments have shown that escalating viral virulence in response to increases in host resistance is not unique to MYXV in Australia. In a remarkable case of parallel evolution, the same thing happened in Europe after a different strain of MYXV was released for rabbit control following the Australian successes. Wild rabbits became more resistant over time, and field isolates of the virus ramped up in virulence. Viral strains isolated in the U.K. around 2010 even caused hyper-immunosuppression in lab rabbits, just like the viruses that had evolved earlier in Australia.6
NASTY PATHOGENS: Infections that circulate among wild animals, such as the myxoma virus in rabbits or the bacterium Mycoplasma gallisepticum in house finches, tend to increase in virulence as hosts develop resistance. If the same holds true for farmed animals, there’s concern that breeding and vaccination efforts aimed at increasing host resistance could fuel the evolution of more virulent pathogens. Chris Cairns (bottom, left) and Andrew Read of Penn State University are studying this phenomenon, pictured here sampling broiler chickens for Marek’s disease virus in central Pennsylvania.RABBIT: PETER KERR; FINCH: BOB VUXINIC; CHICKENS: ASHLEY CHANCommon garden experiments have shown that escalating viral virulence in response to increases in host resistance is not unique to MYXV in Australia. In a remarkable case of parallel evolution, the same thing happened in Europe after a different strain of MYXV was released for rabbit control following the Australian successes. Wild rabbits became more resistant over time, and field isolates of the virus ramped up in virulence. Viral strains isolated in the U.K. around 2010 even caused hyper-immunosuppression in lab rabbits, just like the viruses that had evolved earlier in Australia.6
And it’s not just MYXV. Few diseases have been subject to the scale of common garden experimentation that Fenner and colleagues lavished on MYXV (these studies are not easy or cheap), but escalating virulence in response to naturally selected host resistance seems to have occurred wherever researchers have looked for it. For instance, in the late 1990s, highly lethal rabbit hemorrhagic disease virus (RHDV) escaped from quarantine while Australian authorities were investigating it as a possible biocontrol agent against rabbits. It, too, decimated wild rabbit populations, which consequently evolved resistance against RHDV. In turn, even more virulent viruses evolved.7 Similarly, the mosquito-borne West Nile virus (WNV) spread across the U.S. after first appearing in New York in 1999. It infects a wide range of hosts, including humans, but its core reservoir is wild birds. House sparrows have become more resistant through time, and the virus has correspondingly become more virulent.8
See “A Race Against Extinction”
Virulence also increased after a bacterial pathogen of poultry, Mycoplasma gallisepticum (MG), jumped into the Eastern US house finch population sometime in the mid-1990s. In house finches, MG causes severe conjunctival inflammation that affects over-winter survival. When it first emerged, house finch populations declined by up to 60 percent. Over the subsequent 15 years, MG virulence increased. In the early 2000’s, a relatively low-virulence strain of MG established itself in Pacific house finch populations, and the same thing happened again: virulence increased through time. On both sides of the continent, these increases occurred as partially immune survivors became common in finch populations.9
Thus, nasty pathogens of birds and mammals evolved to become even nastier following six separate emergence events on three continents. Importantly, these six cases cover a diversity of pathogens, including a large DNA virus (MYXV), small single-stranded RNA viruses (RHDV and WNV), and a bacterium (MG). For two of these (MYXV and MG), virulence increases occurred on two separate occasions. The quality of the evidence that the changes in pathogen virulence was caused by rising resistance in the hosts varies, but it is hard to imagine in any of these cases that the increasingly virulent strains could have much of an evolutionary future in highly susceptible hosts, which would likely die before the infectious agent could be transmitted. In all likelihood, the hosts had gained sufficient resistance to ensure somewhat prolonged infectious periods for the more virulent strains. We know of no cases where controlled experiments have shown declines in pathogen virulence in the face of rising host resistance.
Implications for agriculture
Enhancing the resistance of farm animals to infectious disease is an aspiration of veterinary medicine and most agricultural industries, not least because intensive farming is only possible if infectious diseases can be controlled. Traditional selective breeding, genetic engineering, and immunization can all be used to make animals more resistant to infections. If pathogens in nature respond to increases in host resistance by evolving greater virulence, however, is it possible that such efforts will unintentionally select for the same response in pathogens infecting farm animals?
Nothing will happen if hosts are made completely resistant: stop onward transmission, and evolution will cease as well. But artificially enhanced resistance is often imperfect. Many vaccines used on farms do not render hosts impervious to infection, and animal breeders have yet to produce animals completely resistant to a number of different infections. In those situations, pathogens will evolve in newly resistant hosts, just as MYXV, RHDV, WNV, and MG did. Given what we now know about pathogen-host arms races, we think we have to take seriously the possibility that by creating resistant hosts, humans might trigger the evolution of more-virulent animal pathogens.
In fact, this may have already happened. Marek’s disease virus (MDV) is a highly contagious cancer-causing herpesvirus of poultry. Fenner-style common garden experiments clearly show that MDV has become more virulent over the last 50 years.10 When the poultry industry began to ramp up in the 1950s, MDV caused mild disease and had little economic impact. Currently, MDV strains that kill all unvaccinated birds in just 10 days are common in the US and Europe. Birds have to be vaccinated or the losses are devastating. Critically, and for reasons not fully understood, MDV vaccines protect against disease but they do not generate so-called sterilizing immunity: vaccinated hosts can become infected and transmit viruses to other chickens.
The best bird would be one that dropped dead as fast as possible, before it has started transmitting virus to other birds.
In a series of experiments with strains of varying virulence, one of us (AR), together with Venu Nair and colleagues at the Pirbright Institute in England, found that the hypervirulent, or “hot,” strains of MDV that dominate nowadays can exist only in vaccinated flocks. In unvaccinated birds, they kill before they have a chance to be transmitted. Vaccines keep birds infected with the hot strains alive and so massively increase their transmission potential.11 We can’t know for sure that vaccination caused the evolution of the hot strains in the first place (sadly, no Fenner-equivalent experiments tracked the initial evolution), but we can say that without vaccination, there would be no hot strains: vaccination creates the conditions for hot strains to emerge and persist.
We can’t help but wonder if something similar is happening in other poultry diseases. Highly pathogenic strains of several viruses—most notably, those that cause infectious bursal disease, avian influenza, and Newcastle disease—arise from circulating strains that are less virulent. The resulting outbreaks can be economically devastating. In all those cases, vaccines are available and often widely used. But none of the vaccines generate sterilizing immunity. We think it should be a top priority to determine whether, by reducing bird fatalities and hence the death rates of hypervirulent strains, vaccines are actually increasing the risk of outbreaks of highly pathogenic avian influenza in birds.
In addition to vaccination, breeding companies that raise poultry and other livestock often try to use selective breeding to enhance resistance. For example, particular major histocompatibility complex alleles in poultry reduce the severity of disease caused by Marek’s disease virus, and there are concerted efforts to spread those alleles through national flocks. This breeding, as well as the increasing development of genetically engineered resistance,12 may further encourage the evolution and spread of virulent strains. For instance, transgenic chickens have recently been constructed that suppress the replication and transmission of avian influenza, but don’t block it entirely.13 This is directly analogous to the antiviral effects of MYXV resistance that arose in Australia’s rabbits. Were such chickens to go into widespread use, it is easy to imagine that, just like the rabbits in Australia, they would cause the evolution of more-virulent viruses.
Our suggestion is that breeders and engineers try to do the reverse: breed for susceptibility. The best bird would be one that dropped dead as fast as possible, before it has started transmitting virus to other birds. If death can’t be arranged, engineer an animal that becomes obvious to a farmer on first infection—perhaps something as dramatic as a change of color, which could be monitored by cameras—so it can be removed from the flock before it starts an outbreak. Convincing the industry to employ such a counterintuitive strategy will undoubtedly be difficult, of course.
Moreover, virulence is defined in a standardized host, often one that is fully susceptible. If industrial animals are made more resistant, it may not matter if pathogens become more virulent in response. The threat only exists for those animals that remain susceptible.
For example, there is absolutely no question that MDV has become substantially more virulent over the last 50 years, but industry losses to Marek’s disease are nothing like they were when less virulent strains circulated.14 One reason is that in vaccinated birds, even today’s hypervirulent strains cause less-severe disease than did milder strains in unprotected birds. Current viral strains only cause problems when they get into unvaccinated flocks—for example, some organic operations, small outdoor flocks, or production systems with faulty vaccination practices. And that’s the rub.
This issue may be of particular concern when it comes to aquaculture, where not all operations in a particular watershed might have access to vaccines or genetically resistant fish stock, and nearby wild populations might be very vulnerable.15 Likewise, it is easy to envisage non-GMO poultry operations being threatened by hypervirulent pathogens evolving in flocks engineered for resistance. An ethically challenging possibility is that companies deploying resistance-enhancing technologies might gain twice: protection for their own animals and the creation of pathogens that could put their competitors out of business.
Planning for the future
Emergent wildlife diseases show that increasingly aggressive pathogens can attempt to overcome novel host resistance mechanisms as they arise. In the case of MYXV, it is unclear what the very long-term outcome of the escalating arms race will be. But so long as there is virus around, there is no going back: less-resistant hosts would, like our experimental animals, be hugely vulnerable to the hypervirulent viruses now circulating. So, what is the lesson in all this for animal breeders, genetic engineers, and vaccine developers? As in politics and war, if you plan to escalate, also plan for escalation by your opponent.
|
PUBLIC HEALTH Could the widespread use of human vaccines lead to the evolution of pathogens that would be more harmful to the unvaccinated? Most of the human vaccines that have been in use for decades generate sterilizing immunity and so would not be expected to promote pathogen evolution. But next-generation vaccines might be less effective. Clearly, we all hope for malaria or HIV vaccines that completely prevent transmission, but in the absence of fundamental breakthroughs, it seems likely that our current list of vaccine-preventable diseases will soon be joined by a list of vaccine-ameliorable diseases, in which symptoms are alleviated but infection and onward transmission continue. In those cases, it will be critical to understand the possible evolutionary trajectories those target pathogens might take once they evolve in populations that can, just like resistant Australian rabbits, control pathogen titers and sickness, but not prevent infection.
Mathematical models and experimental studies point to the possibility that for some diseases and some vaccines, immunized people might create conditions for the evolution of pathogens that cause more-severe disease in the nonimmunized.1,2 There are controversial suggestions that this might already be so for the nonsterilizing vaccines against pertussis (also known as whooping cough),3,4,5 and for our money, there is a strong case for examining the evolutionary consequences of vaccines against cervical cancer and typhoid fever. This is not an argument against next-generation vaccines; rather, it is an admonition that, in the future, we may need additional tools to protect those whom vaccines cannot reach. |
Andrew F. Read is an evolutionary microbiologist at Penn State’s Center for Infectious Disease Dynamics. Peter J. Kerr is a virologist and honorary fellow at the Marie Bashir Institute for Infectious Diseases and Biosecurity at the University of Sydney.
References
- F.N. Ratcliffe et al., “Myxomatosis in Australia: A step towards the biological control of the rabbit,” Nature, 170:7-11, 1952.
- F. Di Giallonardo, E.C. Holmes, “Viral biocontrol: Grand experiments in disease emergence and evolution,” Trends Microbiol, 23:83-90, 2015.
- B. Cooke et al., “The economic benefits of the biological control of rabbits in Australia, 1950–2011,” Aust Econ Hist Rev, 53:91-107, 2013.
- F. Fenner, B. Fantini, Biological Control of Vertebrate Pests (Wallingford, U.K: CABI Publishing, 1999).
- P.J. Kerr et al., “Next step in the ongoing arms race between myxoma virus and wild rabbits is a novel disease phenotype,” PNAS, doi:10.1073/pnas.1710336114, 2017.
- P.J. Kerr et al., “Genomic and phenotypic characterization of myxoma virus from Great Britain reveals multiple evolutionary pathways distinct from those in Australia,” PLOS Pathog, 13:e1006252, 2017.
- P. Elsworth et al., “Increased virulence of rabbit haemorrhagic disease virus associated with genetic resistance in wild Australian rabbits (Oryctolagus cuniculus),” Virology, 464:415-23, 2014.
- N.K. Duggal et al., “Evidence for co-evolution of West Nile virus and house sparrows in North America,” PLOS Negl Trop Dis, 8:e3262, 2014.
- D.M. Hawley et al., “Parallel patterns of increased virulence in a recently emerged wildlife pathogen,” PLOS Biol, 11:e1001570, 2013.
- R.L. Witter, “Increased virulence of Marek’s disease virus field isolates,” Avian Dis, 41:149-63, 1997.
- A.F. Read et al., “Imperfect vaccination can enhance the transmission of highly virulent pathogens,” PLOS Biol, 13: e1002198, 2015.
- L. Tiley, “Transgenic animals resistant to infectious diseases,” Rev Sci Tech, 35:121-32, 2016.
- S.J. Byun et al., “Transgenic chickens expressing the 3D8 single chain variable fragment protein suppress avian influenza transmission,” Sci Rep, 7:5938, 2017.
- D.A. Kennedy et al., “An observational study of the temporal and spatial patterns of Marek’s-disease-associated leukosis condemnation of young chickens in the United States of America,” Prev Vet Med, 120:328-35, 2015.
- D.A. Kennedy et al., “Potential drivers of virulence evolution in aquaculture,” Evol Appl, 9:344-54, 2016.
Interested in reading more?




