 © ISTOCK.COM/BLONDIEGIRL/PROFESSORPHOTOSHOP
© ISTOCK.COM/BLONDIEGIRL/PROFESSORPHOTOSHOP
For three consecutive winters, starting in 2011, researchers at the University of Birmingham asked healthy men and women over the age of 65 to come in to clinics across the western Midlands in the U.K. for a seasonal influenza vaccination at specific times of day—either between 9 and 11 a.m., or between 3 and 5 p.m. Blood drawn a month later revealed that participants, who totaled nearly 300 over the three years, had higher levels of anti-flu antibodies if they’d received their vaccinations in the morning.1 The results suggested that daily rhythms of people’s bodies tweaked the vaccine’s effectiveness. Lead author Anna Phillips Whittaker had suspected as much, after observing similar trends in her studies on behavioral factors such as exercise that affect vaccination responses, and in the wake of a growing body of literature suggesting that a little timing can go a long way when...
Many hormones and immune signals are produced rhythmically in 24-hour cycles. Cortisol, for example, which is known to suppress inflammation and regulate certain T cell–mediated immune responses, peaks early in the morning and ebbs as the day progresses. Other facets of the immune system undergo similar cycles that could underlie the differences in antibody responses Phillips observed among people receiving the flu vaccine. Much more work is required to nail down the immune mechanisms responsible for such variation and exploit them appropriately, she says. But timing flu vaccine delivery would be straightforward to implement. “It’s such a simple, low-risk intervention that’s free to do, and could have massive implications for vulnerable populations.”
Now we have the groundwork to precisely understand a person’s clock and leverage that information for better health.—John Hogenesch,
University of Pennsylvania
Across diseases, from cancer and cardiac ailments to allergies and arthritis, epidemiological data and clinical trials are revealing that timing medications to the body’s internal clock could improve their effectiveness and reduce side effects. Although this concept, known as chronotherapy, has existed for at least 60 years, it has received little attention from physicians. But as biologists continue to unveil the molecular intricacies of cellular rhythms, they are beginning to realize just how pervasive the circadian clock’s influence is. In a 2014 study of gene expression in mice, for example, researchers found periodic expression in conserved mammalian genes targeted by 56 of the top 100 best-selling drugs in the U.S., including aripiprazole (Abilify, an antipsychotic), esomeprazole (Nexium, for heartburn), and duloxetine (Cymbalta, for depression), even though most are not currently prescribed with suggested dosing times.2
But chronotherapy is gaining clinical traction, says University of Pennsylvania chronobiologist John Hogenesch, senior author on the 2014 study. “Now we have the groundwork to precisely understand a person’s clock and leverage that information for better health,” he says. “Because of the molecular work, we’ve opened new doors here. This [idea] is not coming from left field anymore.”
Even so, researchers and clinicians working on chronotherapy still face skepticism, and implementing a new drug-delivery protocol or gaining regulatory approval from the US Food and Drug Administration (FDA) for time-of-day indications remains challenging. Thus, while the biomedical research community is starting to take notice of the body’s internal rhythms, timed therapies are still the exception to the rule.
The body’s clock
By the 1970s, experimental data were piling up to support the idea that timing of exposure to toxins, X-rays, or drugs could alter the effects of these agents.3 Researchers found that the rate-limiting enzyme regulating the synthesis of cholesterol in rats was most active at night, for example.4 Within the next few years, researchers were examining cholesterol regulation in humans and testing the effects of administering cholesterol-lowering drugs at different times of day. Short-acting drugs such as simvastatin, which is still prescribed today, are most effective when taken at bedtime.5 Accordingly, the FDA has long recommended taking such medications in the evening.
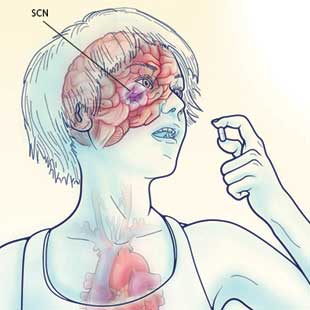 BY DAY OR BY NIGHT: The human body undergoes daily cycles in gene expression, protein levels, enzymatic activity, and overall function. The suprachiasmatic nucleus (SCN), the seat of the brain’s timekeeping machinery, sets the pace for neuronal and hormonal signals that regulate body temperature, feeding behavior, rest or activity, immune cell functions, and other daily activities.
BY DAY OR BY NIGHT: The human body undergoes daily cycles in gene expression, protein levels, enzymatic activity, and overall function. The suprachiasmatic nucleus (SCN), the seat of the brain’s timekeeping machinery, sets the pace for neuronal and hormonal signals that regulate body temperature, feeding behavior, rest or activity, immune cell functions, and other daily activities.
See full infographic: WEB | PDF© EVAN OTO/SCIENCE SOURCEIn the past 20 years, a slew of studies using genetic screens and genome-wide expression analyses have begun to establish the reasons for these and similar observations.6 A group of approximately 20,000 neurons in a region of the hypothalamus called the suprachiasmatic nucleus (SCN) acts as a central timekeeper, while clock genes expressed around the body form self-regulating feedback loops that allow the body to keep time at the level of individual organs, tissues, or cells. Nerve impulses and hormonal cues initiated by SCN activity relay central timing information to peripheral clocks, and external cues including light, mealtimes, or temperature can alter peripheral clocks, which then send feedback to other systems in the body.
See “Go To Bed”
Mounting evidence indicates that keeping the body’s cells synced up matters to the health of an organism. In 2007, based on epidemiological studies, the International Agency for Research on Cancer declared shift work, which causes circadian disruption, a carcinogen. Other studies have elucidated a link between immune cell activity and glucocorticoids—which are secreted in circadian patterns and regulate peripheral clocks—as well as a role for chronic stress in perturbing daily cycles in gene expression, which can alter immune, endocrine, and other functions.7 This more precise knowledge is beginning to infiltrate the clinic, finally coming to the aid of physicians trying to more effectively time therapeutic interventions.
“There are thousands of studies since the 1970s, but little of that work was done in a mechanistic fashion,” says Hogenesch. “Now we have a relatively complete picture of clock networks across the organism, and we can see actual genetic targets that are oscillating, so we can begin investigating the mechanisms underlying those observations.”
Timing for tumors
Genes involved in cell division were among the earliest identified as being rhythmically expressed in both rodent models and human cells. In 1987, researchers studying ovarian cancers found that tumor cells synthesized DNA on a daily rhythm that typically peaked in the late morning hours, nearly 12 hours out of sync with nontumor cells.8 This led the team to suggest that timing chemotherapy doses that target cells actively replicating their DNA might improve the drugs’ effectiveness while reducing healthy-cell death.
 TIMING TREATMENTS TO THE CLOCK: Regulated by peripheral clocks and interactions with other organs, many metabolic pathways in the body peak and ebb in specific circadian patterns. As a result, drugs targeting these pathways can work better when taken at particular times of day. Here are a few examples.
TIMING TREATMENTS TO THE CLOCK: Regulated by peripheral clocks and interactions with other organs, many metabolic pathways in the body peak and ebb in specific circadian patterns. As a result, drugs targeting these pathways can work better when taken at particular times of day. Here are a few examples.
See full infographic: WEB | PDF© EVAN OTO/SCIENCE SOURCE
Sure enough, over the past 30 years, experimental models and clinical trials have found that timing chemo regimens can significantly affect their toxicity and effectiveness. In animal studies of nearly 30 chemo drugs, tailoring dosing time to the medication’s mode of action has been found to decrease toxic side effects and increase effectiveness. In one study, rats that received the chemotherapy drug cisplatin at the time of day when their urinary output was highest (a correlate of other timed cycles in kidney metabolism) had fewer nephrotoxic effects, as measured in kidney function tests, than animals that received the doses at the time of minimum urinary output.9 In another study, oxaliplatin chemotherapy caused fewer intestinal lesions and less bone marrow suppression in mice when given at night, possibly because DNA synthesis in murine bone marrow is highest during the day.10
Because rodents are nocturnal, however, the appropriate schedule changes as the experiments move into humans. And timing drug administration becomes even more complicated when patients are treated with combination therapies. But researchers are seeing success in human studies testing chronotherapy for cancer. In multiple clinical trials, they have found that patients with ovarian, endometrial, or metastatic bladder cancer who received doxorubicin at 6:00 a.m. and cisplatin 12 hours later experienced less toxicity and greater tumor response and survival than those who received the drugs in the reverse sequence.11 Oncologist and biomedicine professor Francis Levi, a pioneer of chronobiology research now at the University of Warwick, has also shown repeatedly that patients experience better responses and fewer side effects from toxicity when drugs are administered at specific times of day.12 “At this point we have conducted about 30 clinical trials,” he says. “We have found that chronotherapy can improve survival up to fivefold and shrink tumors twice as much when compared to conventionally administered chemotherapy.”
But circadian-timed chemotherapy only shows benefits for approximately half of patients in trials, Levi notes. One possible influence is gender, he says. In a meta-analysis of data from three Phase 3 trials, he and his colleagues found that nighttime chemotherapy improved survival in men but not women.13 Phillips has also noticed gender-specific effects in studies of morning versus afternoon vaccinations, but only in younger populations, not among the elderly, so age may also play a role.
Another factor could be genetics. In 2014, a group of Israeli scientists found that in mice, glucocorticoid signaling—mediated by hormones that peak at night and taper off in the morning—suppressed levels of epidermal growth factor receptor (EGFR), which has been linked to tumor growth and migration. EGFR signals were stronger during the day when glucocorticoid levels were lowest; correspondingly, tumors in mice that were driven by EGFR mutations grew faster at this time. An EGFR inhibitor used to treat breast cancer slowed tumor growth more when given to the animals in the daytime than when the same dose was administered at night.14
The core clock genes themselves may also differ among individuals. In wild-type mice, researchers found a timing-dependent response to the chemo drug cyclophosphamide, but they also found that animals lacking a circadian rhythm because of mutations in the clock genes BMAL1 and CLOCK did not show a time-dependent response.15 Another study by Levi and colleagues, using circadian gene expression data for 27 genes from mouse liver and human colon cancer cell lines, found that the optimal time to administer the chemotherapy agent irinotecan could be predicted based on a gene regulatory loop controlled by clock genes BMAL1 and REV-ERBα. When BMAL1 was silenced in vitro, irinotecan’s timing-dependent effects vanished.16
Whatever the cause of the variation, researchers must now deal with it in a systematic way, Levi says. “Until a few years ago, our working hypothesis was to deliver chronotherapy to an average rhythmic pattern in a population, so all patients receive the exact same protocol,” he says. “But interpatient differences could result in a marked improvement in some cases and none in others. This clearly indicates that we need to identify individual rhythms, analogous to what we’re doing in personalized medicine now.” (See “Getting Personal,” The Scientist, February 2017.)
Clocking other conditions
Even as chronotherapy was gaining recognition in the oncology research community, investigators realized that cancer was not the only disease likely to be affected by circadian cycles. Clinical trials in 1985 found that antihistamines were most effective when taken at night or early in the morning. Subsequent studies established that inhaling corticosteroids at bedtime, or using delayed-release prednisone formulations that allocated the medication to the body pre-dawn, were most effective at combating allergy symptoms.17 Cardiovascular events were also recognized early on to cycle throughout the day, as doctors noticed that most patients admitted for heart attacks tended to experience their symptoms between 6:00 a.m. and noon.18
Across diseases, from cancer and cardiac ailments to allergies and arthritis, epidemiological data and clinical trials
are revealing that timing medications to the body’s internal clock could improve their effectiveness and reduce side effects.
More recently, researchers have begun to capitalize on the body’s link to the clock. In 2009, for example, after finding that blood pressure declines at bedtime and starts to rise early in the morning—in part because the angiotensin-2 receptor is maximally expressed at night—scientists discovered that patients with high blood pressure were better able to control their blood pressure and cardiovascular symptoms by taking angiotensin receptor blockers at night instead of in the morning.19
But the benefits of a bedtime dose don’t extend to all blood pressure medications, St. Louis College of Pharmacy’s Amy Drew points out. In 2014, pulling data from approximately 30 studies, Drew and her colleagues evaluated a range of hypertension medications for time-dependent effects. While angiotensin-2 receptor blockers were significantly more effective if taken at bedtime, other drugs, such as certain calcium channel and β-adrenergic blockers, didn’t seem to have a clear benefit from being administered at a particular time of day.20 Some treatments have a diuretic effect, which might disturb patients’ sleep and make the medicine less effective, Drew says.
Nevertheless, the data for a time effect of angiotensin-2 receptor blockers is compelling, she adds. “Going through all this evidence, it allows you a certain comfort and confidence to say that if I do dose [angiotensin-2 receptor blockers] at bedtime, it’s going to be more effective.”
Implementing chronotherapy
 © KUDRYASHKA/SHUTTERSTOCK.COM; ISTOCK.COM/RHOON
© KUDRYASHKA/SHUTTERSTOCK.COM; ISTOCK.COM/RHOON
Synchronizing medications to the circadian clock is easier said than done, as not everyone’s rhythms are the same. And for patients who suffer poor sleep, reduced appetite, or fatigue that reduces their physical activity—common symptoms of many diseases—the clock itself often runs awry.
Researchers are now working to figure out how to normalize patients’ circadian rhythms. In a small study of 32 patients with metastatic breast cancer, over-the-counter melatonin—often used to cope with jet lag or insomnia—was found to improve sleep quality and morning expression of circadian genes.21 And preliminary results from an ongoing trial at Mount Sinai Hospital in New York suggest that exposure to bright white light can reduce disease-related fatigue in patients with breast cancer.22
Psychosocial support may also prove beneficial. In 1989, Stanford University psychiatrist David Spiegel and his colleagues reported that women with breast cancer who participated in group therapy sessions lived an average of 18 months longer than patients who didn’t receive psychosocial support to cope with their diagnosis.23 Spiegel’s team reported in a follow-up study that the effect was likely mediated by the endocrine stress response; when levels of cortisol followed a normal curve, cresting in the morning and ebbing by nightfall, patients lived longer.24 In 2012, another group reported that breast cancer patients who received eight weeks of group therapy were more likely to have improved diurnal cortisol rhythms than those who received a single educational session.25
“We’ve learned enough now to know that there are relatively easy-to-do, low-risk things that may have an effect on disease outcomes,” Spiegel says. “If you normalize your circadian rhythms, you’ll certainly feel better, and you might just help your body,” he adds. “I’d be surprised if there were any disease that didn’t have some circadian component.”
The trick now is to understand how time of day affects disease outcomes and treatment effects, and to respond accordingly—which may not be a slam dunk, says Hogenesch. “Many of these observations are in the scientific literature but not on drug labels.” He and others aim to change that, beginning with the clinical trials necessary to demonstrate daily variations in a drug’s effectiveness. A little timing could even rescue drugs that fell off the path to the clinic somewhere along the way, says Hogenesch, who consults with drug companies interested in putting chronotherapy into practice. “In the past when trials were done, time-of-day information was often not captured. It’s very likely that drugs have failed not because they didn’t work or the mechanisms were wrong, but simply because time of administration wasn’t taken into account.”
To chronobiologists, time is an often-overlooked aspect of precision medicine’s mantra of finding the right drug for the right patient at the right dose. “The discussion is almost entirely focused on genetic precision, and not on all these aspects of physiology and behavior that are products of [the circadian] genetic network,” says Hogenesch. “Time offers another way to be precise, and now the groundwork exists to precisely understand a person’s clock and leverage that information for better health.”
Jyoti Madhusoodanan is a freelance writer based in San Jose, California.
References
- J.E. Long et al., “Morning vaccination enhances antibody response over afternoon vaccination: A cluster-randomised trial,” Vaccine, 34:2679-85, 2016.
- R. Zhang et al., “A circadian gene expression atlas in mammals: Implications for biology and medicine,” PNAS, 11:16219-24, 2014.
- F. Halberg et al., “Toward a chronotherapy of neoplasia: Tolerance of treatment depends upon host rhythms,” Experientia, 29:909-34, 1973.
- P.A. Edwards et al., “In vivo demonstration of the circadian rhythm of cholesterol biosynthesis in the liver and intestine of the rat,” J Lipid Res, 13:396-401, 1972.
- R.H. Knopp, “Drug treatment of lipid disorders,” New Engl J Med, 341:498-511, 1999.
- J.A. Mohawk et al., “Central and peripheral circadian clocks in mammals,” Annu Rev Neurosci, 35: 445-62, 2012.
- R. Dumbell et al., “Circadian clocks, stress, and immunity,” Front Endocrinol, 7:37, doi:10.3389/fendo.2016.00037, 2016.
- R.R. Klevecz et al., “Circadian gating of S phase in human ovarian cancer,” Cancer Res, 47:6267-71, 1987.
- F.A. Levi et al., “Reduction of cis-diamminedichloroplatinum nephrotoxicity in rats by optimal circadian drug timing,” Cancer Res, 42:950-55, 1982.
- N. Boughattas et al., “Circadian rhythm in toxicities and tissue uptake of 1,2-diaminocyclohexane oxalatoplatinum in mice,” Cancer Res, 49:3362–68, 1989.
- M. Kobayashi et al., “Circadian chemotherapy for gynecological and genitourinary cancers,” Chronobiol Int, 19:237-51, 2002.
- F. Lévi et al., “Implications of circadian clocks for the rhythmic delivery of cancer therapeutics,” Adv Drug Deliv Rev, 59:1015-35, 2007.
- S. Giacchetti et al., “Sex moderates circadian chemotherapy effects on survival of patients with metastatic colorectal cancer: A meta-analysis,” Ann Oncol, 23:3110-16, 2012.
- M. Lauriola et al., “Diurnal suppression of EGFR signalling by glucocorticoids and implications for tumour progression and treatment,” Nat Comm, 5:5073, doi:10.1038/ncomms6073, 2014.
- V.Y. Gorbacheva et al., “Circadian sensitivity to the chemotherapeutic agent cyclophosphamide depends on the functional status of the CLOCK/BMAL1 transactivation complex,” PNAS, 102:3407-12, 2005.
- S. Dulong et al., “Identification of circadian determinants of cancer chronotherapy through in vitro chronopharmacology and mathematical modeling,” Mol Cancer Ther, 14: 2154-64, doi:10.1158/1535-7163.MCT-15-0129, 2015.
- F. Buttgereit, A. Gibofsky, “Delayed-release prednisone – A new approach to an old therapy,” Expert Opin Pharmacother, 14:1097-106, 2013.
- J.E. Muller et al., “Circadian variation in the frequency of onset of acute myocardial infarction,” New Engl J Med, 313:1315-22, 1985.
- R.C. Hermida et al., “Administration-time-dependent effects of olmesartan on the ambulatory blood pressure of essential hypertension patients,” Chronobiol Int, 26:61-79, 2009.
- P.M. Stranges et al., “Treatment of hypertension with chronotherapy: Is it time of drug administration?” Annals of Pharmacotherapy, 49:323-34, 2015.
- P.F. Innominato et al., “The effect of melatonin on sleep and quality of life in patients with advanced breast cancer,” Support Care Cancer, 24:1097-105, 2016.
- W.H. Redd et al., “Systematic light exposure in the treatment of cancer-related fatigue: A preliminary study,” Psycho-Oncology, 23:1431-34, 2014.
- D. Spiegel et al., “Effect of psychosocial treatment on survival of patients with metastatic breast cancer,” Lancet, 334:888-91, 1989.
- S.E. Sephton et al., “Diurnal cortisol rhythm as a predictor of breast cancer survival,” J Natl Cancer Inst, 92:994-1000, 2000.
- F.-H. Hsiao et al., “The effects of psychotherapy on psychological well-being and diurnal cortisol patterns in breast cancer survivors,” Psychother Psychosom, 81:173-82, 2012.
Interested in reading more?




